
Traditional Medicare or an Advantage Plan?
Medicare Advantage or traditional Medicare with supplemental insurance: which should you choose?
A compelling reason so many 65-year-olds are flocking to Medicare Advantage insurance policies is that they tend to have significantly lower premiums than enrolling directly in traditional Medicare. Retirees are also inundated with advertisements on television, online and in the mail urging them to sign up for the Advantage plans, which sometimes cover vision and dental care.
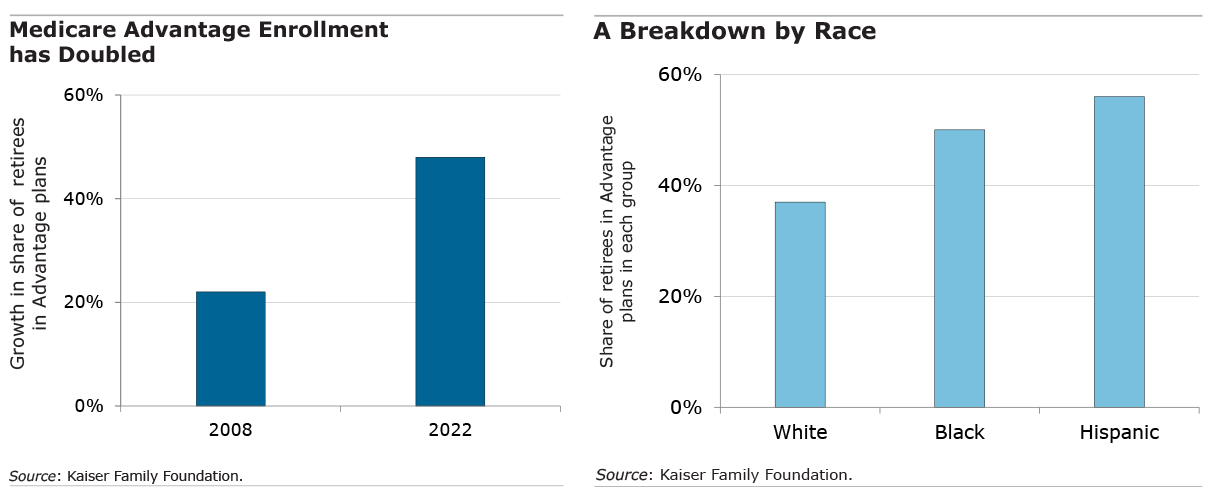
But the premium alone is a superficial test for such a consequential decision. Traditional Medicare plans combined with a Medigap or Part D drug plan might, in the end, be less costly. Differences in the quality of care and the out-of-pocket costs can weigh more heavily over the long haul as retirees get older and their health declines.
The federal government spent $321 more per person in 2019 on Medicare benefits in Advantage plans than on each person enrolled directly in traditional Medicare, according to Kaiser. “The growing role of Medicare Advantage and the relatively high spending on this program raise the question of how well private plans serve their enrollees,” Kaiser said.
To shed light on the advantages and disadvantages of each route, Kaiser’s researchers combed through more than five dozen academic studies and packaged them into a report comparing the care provided under Medicare Advantage policies and traditional Medicare.
Kaiser, a healthcare non-profit, found that both choices had some important things in common, including similar levels of patient satisfaction with care, wait times, care coordination, and the ability to find a doctor or specialist.
Medicare Advantage plans are separate insurance policies, and the federal government pays the insurance company for some of the care. Traditional Medicare in this report covers people who pay the federal Medicare premium for Part A and B coverage, and people who enroll in Medicare and also buy a Medigap supplement or Part D drug policy from an insurer.
A decision made at 65 isn’t irreversible. But most retirees tend to stay put once they choose between an Advantage insurance policy and traditional Medicare. It’s also important to remember that migrating from a Medicare Advantage policy to a Medigap supplement is more difficult than going from Medigap to Medicare Advantage.
Here’s a rundown of the most salient differences in cost and care in Kaiser’s summary. But this is a complicated decision, and many of the findings are subtle. So read the full report to understand the nuances.
Cost. The cost of medical care is crucial for millions of retirees on a tight budget and has an impact on the quality of care: retirees say they skip or delay care deemed unaffordable. Medicare Advantage plans with low or no premiums are definitely a cost saver upfront since premiums make up the biggest share of lifetime medical costs. But in addition to premiums, out-of-pocket costs go toward doctor visits, tests, prescriptions, and copayments for hospital or other care.
When 65-year-olds are deciding between Advantage plans and traditional Medicare, it may come down to this tradeoff: lower premiums now versus the risk of having to pay more over a lifetime. Kaiser cited studies showing that retirees enrolled directly in traditional Medicare, either by itself or with a supplemental policy, have slightly fewer problems paying for care than people with Advantage policies. This also was the case in separate cost studies for Black Americans, people in poor health, and people under 65 with disabilities.
Another way to look at cost is the risk that retirees might be socked with inordinately high medical costs if they develop a serious illness. One study not covered in the Kaiser report found that 23 percent of retirees with Advantage plans had out-of-pocket costs, excluding premiums, that exceeded 10 percent of their income, compared with 17 percent of Medigap buyers.
Consistent source of medical care. Consistently receiving medical care from the same doctor or clinic is one way patients can ensure they are getting quality and continuity in their care. Medicare Advantage plans have a slight edge here in a couple of studies. This also held true in studies of specific populations: retirees, people of color, and adults of all ages with severe disabilities.
Other aspects of Advantage plan care had poorer results. Retirees with these plans reported that it was more difficult to get the care they need in three large states: New York, Florida, and California. Advantage plans’ end-of-life care also didn’t stack up as well in surveys with friends and family of the deceased to the care provided in traditional Medicare.
Preventive services. Advantage policies did well in this category. Customers in these plans have higher vaccination rates for flu, more routine checkups and wellness visits, and more thorough screenings for colorectal cancer, breast cancer, and blood pressure.
Avoidable hospital admissions. Admissions are considered to be avoidable if the medical problem had been managed properly by a primary care physician, though the health of the patient is always a factor in whether treatment is successful. One study of Black patients that took patient health into account found that the retirees in Advantage Plans had more potentially avoidable admissions than the retirees enrolled directly in traditional Medicare.
Hospital quality. In two different studies, people with traditional Medicare got care in higher-quality hospitals for non-emergency admissions, though this wasn’t the case in a study of rural hospitals. Traditional Medicare also tended to deliver better quality in cancer care, home health care, and skilled nursing facilities.
Hospital readmissions. Several studies of different patient groups, including Wisconsin residents over 65 and patients discharged from hospitals to skilled nursing facilities, showed that retirees with Advantage plans had lower readmission rates than retirees in traditional Medicare.
However, there were no differences in readmissions between the two coverage options for five medical conditions: heart attack, pneumonia, heart failure, stroke, and hip or knee surgery. Regardless of the type of plan involved, some groups faced a higher risk of being readmitted within 30 days of being discharged: Black surgery patients and patients in skilled nursing facilities.
Post-acute hospital care. Numerous studies found that retirees with Medicare Advantage plans spent fewer days in post-acute care in nursing homes and in-patient rehabilitation centers than retirees with traditional Medicare. Use of home health care was also lower in Advantage plans. Sicker patients with these plans also spent less time in the hospital.
The best advice for retirees enrolling in Medicare is to do the research to understand what you’re buying. Start with the State Health Insurance Assistance Program (or SHIP). There’s one in every state with a staff and volunteers who know the ins and outs of retiree health insurance and can help retirees make smart decisions.
Squared Away writer Kim Blanton invites you to follow us on Twitter @SquaredAwayBC. To stay current on our blog, please join our free email list. You’ll receive just one email each week – with links to the two new posts for that week – when you sign up here. This blog is supported by the Center for Retirement Research at Boston College.
Comments are closed.




![iStock-910619648 [Converted]](https://crr.bc.edu/wp-content/uploads/2023/04/iStock-910619648-Converted-640x454.png.webp)
![shutterstock_547594507 [Converted]](https://crr.bc.edu/wp-content/uploads/2023/03/shutterstock_547594507-Converted-548x480.png.webp)

I was surprised that you didn’t mention the fact that Advantage folks have to stay within “their” system. As opposed to “regular Medicare” folks can go to any hospital or physician they want (instate or not). I think that is an important difference.
Well done. Thanks. I have Medicare Advantage through Kaiser Permanente – very good health and medical care – terrible bureaucracy – lots of waste of Medicare dollars.
Thanks. This is an important report, useful to those approaching 65.
I started out with original Medicare at 65 with AARP Supplement. I switched over to AARP/United Healthcare Medicare Advantage three years ago with zero premium when I was 75. Overall costs have gone down for me, particularly prescriptions. No change in doctors or care. It is working for me.
I’d love to see a report that follows two patients through their care for nearly identical problems. One patient with Medicare, the other with Advantage.
I’ve spent hours comparing Medicare and Advantage policies and could not get clarity about which choice was best.
One key factor for me in selecting the original Medicare is its portability and the fact that I can go to any doctor or specialist without prior approval;I don’t have to select an “in-network” provider. I believe that if I get seriously ill, I am better off with original Medicare and the Medigap, which covers the “excess charges.” With a Medicare Advantage plan, you won’t find out how much out of pocket money you have to spend until you get really sick (if you do). I agree it’s important to spend the time and effort to understand the nuances of both choices. It doesn’t help that the Medicare Advantage plans spend huge dollars on marketing that make it look like an easy choice. It’s a case of “let the buyer beware…” So we’re essentially on our own. The article underscores the importance of using SHIP, and I agree, that is a great first step.
Our readers’ actual experiences with Medicare provide so much valuable information for everyone else. Thanks for pitching in!
When I turned 65 last year, I enrolled in original Medicare, and my former employer’s health plan became the secondary plan. Now, my former employer, a large union, has informed me that starting in January I will automatically be switched to a Medicare Advantage plan. Do I have any recourse? I don’t want to give up original Medicare. Among the new plan’s provisions, if a physician has opted out of Medicare, I will be on the hook for the entire fee. Right now, my secondary plan–UnitedHealth–pays 20% of my out-of-pocket expenses.
That’s really disappointing that you are being forced to make that change. I live in FL, so every provider takes Medicare but that might not be the same in all areas of the country. I think your union is the only entity who can answer your question. If you opt out, will you get a monthly payment from them since they aren’t spending any money on you?