Tag: elderly

Anyone who thinks that moving an elderly parent out of her home and into a facility will eliminate the need for most of the care they’ve been providing should think again. Two University of Pennsylvania researchers added up the hours that adult children, spouses and other unpaid caregivers provide when loved ones are in assisted…
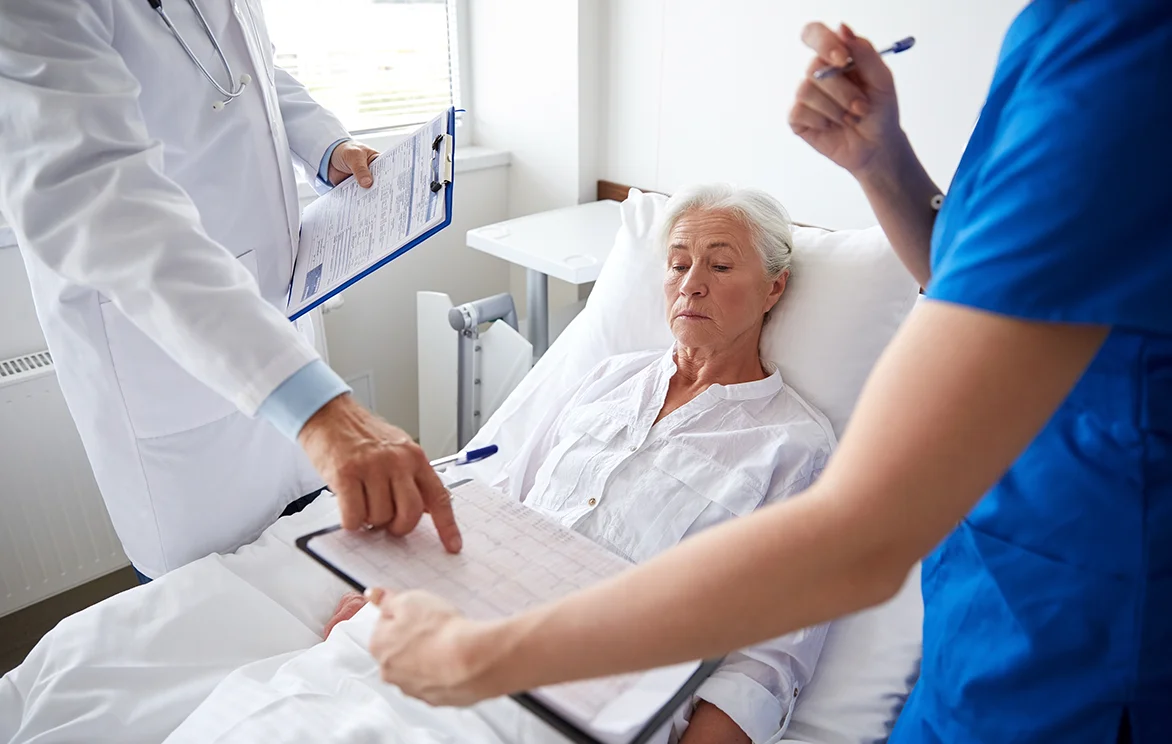
Today’s retirees typically spend about a third less on medical care than retirees did back in 2004, according to new research. Workers who are over 55 but not yet eligible for Medicare are spending somewhat less too. Two policies have reversed the trend of years of rising costs: the introduction of Medicare’s Part D prescription…